The first step in getting a grasp on equine anaemia in horses is to forget about everything you know about anaemia in people. In children, seniors and menstruating women, iron deficiency due to inadequate intake and/or high blood loss is a common cause of human anaemia, but it is virtually non-existent in horses.
Equine anaemia is one of the most commonly misdiagnosed problems in horses, so understanding the possible causes is crucial.
What are the common causes of equine anaemia?
Contrary to the propaganda that some companies throw our way (e.g. the heavily marketed faecal occult blood test for horses), gastrointestinal disease severe enough to cause blood loss equine anaemia is also extremely rare in horses, except for heavily parasitised young foals that have low iron stores in the first place.
It’s questionable if even very severe, high-grade ulcer disease could cause anaemia – and it certainly wouldn’t without there also being correspondingly severe colic.
Low levels of the hormone EPO from advanced kidney disease is a common cause of anaemia in humans and even small animals but kidney failure is very rare in horses and when it does occur is typically at a very advanced stage and not treated as a rule.
Cancer and chemotherapy is another common human cause, not an issue in the horse except for the rare instances of a malignancy.
Is iron a factor in equine anaemia?
Where iron comes in as a player in equine anaemia is in relation to oxidative stress in horses.
In chemistry, any reaction that causes an element to lose an electron is an oxidation reaction. The lost ion may be in the form of a hydrogen ion or hydrogen + oxygen. Either way, it creates a very unstable “free radical” (the liberated hydrogen or hydroxyl group) which will damage adjacent structures in an effort to again become stable. Free radicals are often designed with a dot – OH. = hydroxyl free radicals.
The free radicals that are of most concern to the performance horse are the reactive oxygen species generated during exercise and aerobic metabolism.
Aerobic metabolism is the burning of compounds derived from either glucose or fats in the cell’s energy factories, the mitochondria. This process generates hydrogen ions. Anywhere from 0.1 to 2% of hydrogen ions escape along the electron transport chain in the mitochondria and result in the production of O2., superoxide. Superoxide interacts with the superoxide dismutase enzyme to produce either stable oxygen or, in the presence of excess hydrogen ion, hydrogen peroxide.

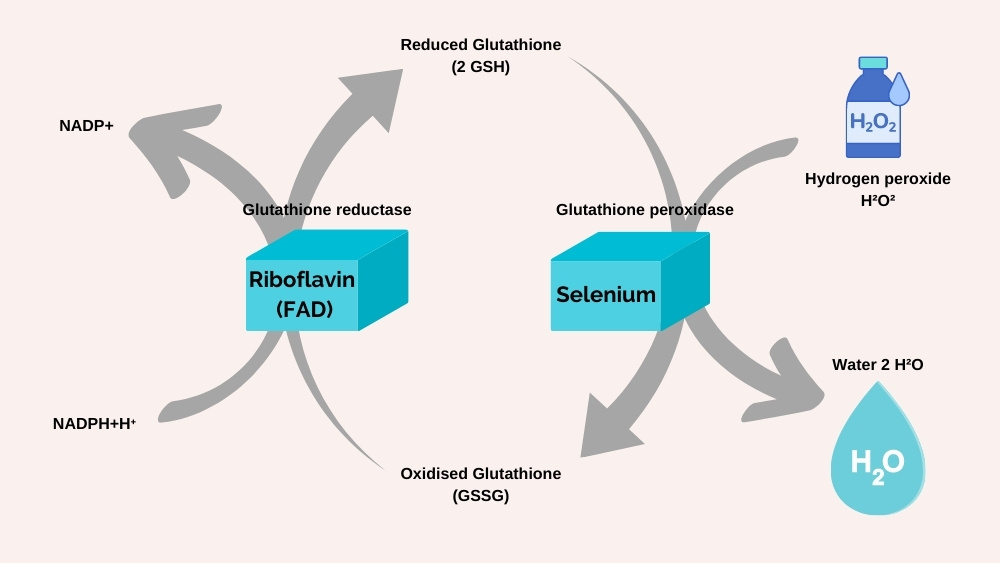
Hydrogen peroxide in turn can break down to produce stable oxygen and OH. radical. Hydroxyl radicals are extremely reactive and will be dealt with by the catalase enzyme which scavenges 4 OH radicals and converts them into two H2O (water) and one O2. Glutathione can also mop up peroxide when it is reduced by the glutathione peroxidase enzyme. This source of free radicals is going on continuously every minute of every day. When the horse exercises, it increases tremendously.
Iron in the body that is not tightly bound to either haemoglobin, a carrier or storage protein is an extremely potent free radical. Red cell membranes are very vulnerable to free radical damage.
How does iron overload affect anaemia in horses?
Iron overload, which can only be diagnosed by the testing panel of serum iron, transferrin and ferritin at the Kansas State University Comparative Hematology Laboratory, can contribute to anaemia in insulin-resistant horses which over absorb iron and in horses over supplemented with iron. Excessive iron supplementation, both orally and intravenously, can also compromise red blood cells and result in low red counts in high-performance horses.
Is anaemia affected by common mineral deficiencies?
Returning to the enzyme systems that protect against oxidative damage to red cells, we can find several areas where common mineral deficiencies can impact the horse’s ability to effectively counteract oxidative stress:
- Copper: Commonly deficient. Copper is at the active mineral center of the superoxide dismutase enzyme. Copper is also critical for the formation of the protein ceruloplasmin, which is required to capture the iron released from old red blood cells and transfer it to the carrier protein, transferrin.
- Zinc: Also an active mineral center for superoxide dismutase.
- Selenium: Critical to the function of glutathione peroxidase enzyme, which mops up peroxide and converts it to water.

An equine anaemia case study
To illustrate how this works, let’s look at the case of a 7-year-old Standardbred racing trotter. He had been given a break because of flagging performance, then slowly reconditioned over a 6 month period. He raced very poorly in his qualifier.
The trainer ran blood work which showed normal red count, hematocrit and red blood cell size but low haemoglobin and low MCHC (mean cell haemoglobin concentration). The only abnormality in his blood chemistry was high indirect bilirubin.
The low haemoglobin looks like iron deficiency, but with iron deficiency, there would also be smaller than normal red cell size. He was feeding the horse Purina grain mixes and a local (Alberta, Canada) timothy hay, no supplements.
The reason for no supplements was that the year before the horse had had a violent allergic reaction (sweating, facial swelling) ten minutes after getting the track vet’s vitamin “jug” (intravenous fluid) that contained B vitamins, iron and vitamin C. Hmmm…..
Other problems the horse had were a dull coat, muscle soreness, occasional EIPH (exercise-induced pulmonary haemorrhage – “bleeder”) and the elevated bilirubin that had been showing up on his blood chemistries for the past year.
Indirect bilirubin is recycled haemoglobin from old red blood cells that have been stripped of its iron. This is bound to albumin in the blood and extracted by the liver.
All things considered, I felt we were dealing with iron overload with deficiencies of vitamin E, selenium, copper and zinc.
The “allergic” type reaction he described I had seen before in iron overloaded horses.
Under conditions of high iron, vitamin C can act as a pro-oxidant (rather than anti), and intravenous iron causes a further burst of oxidative stress. We were unable to get ferritin or ceruloplasmin testing in Canada, so just moved forward on that assumption.
The horse was taken off the commercial compound cereal mixes (which can have 1000 ppm of iron, even more), and put on a mix of 10:35:35:20 peas:oats:corn:alfalfa. This has a nice array of amino acids for muscle support and is balanced in major minerals. He also got vitamin E 5000 IU, 115 grams of flax (micronised linseed), salt, and minerals balanced to his hay with a 4:1 Fe: Cu ratio and 2 mg of selenium. He was put on a 10-day course of both Spirulina and Milk Thistle, to get rapid control of oxidative stress, 30 grams of each twice a day.
It took quite a while to get the minerals lined up, but the switch off commercial cereal compound feeds and on to linseed and vitamin E/selenium alone improved him to the point that he raced third. The big changes came when the minerals went on board. Within 2 weeks, his coat colour darkened and he had much higher energy. He was exercising stronger, with more endurance and speed. Repeat blood work after 6 weeks on the complete diet changes showed:
| Before Diet Change | After Diet Change | Normal | |
| Red count (millions) | 9.21 | 9.09 | 6 to 12 |
| Haemoglobin | 11.4 | 14.1 | 14.5 to 15.5 |
| Mean cell volume | 44 | 44 | 43 to 50 |
| MCHC | 28.1 | 35.5 | 35 to 39 |
Haemoglobin and MCHC took a huge jump, not by supplementing iron but by actually aggressively decreasing it while simultaneously increasing copper for proper iron handling and copper, selenium and zinc to support antioxidant enzyme function. And, of course, the best of all was his first win, which followed soon after.
As mentioned earlier, foals are born with low iron stores and are the only category under normal circumstances where iron deficiency could cause anaemia. Iron is not normally high in milk, but it is very bio-available. There is also strong evidence to suggest that foals need to obtain iron from the environment, specifically soil, to avoid anaemia when young:
J Vet Intern Med. 2001 Sep-Oct;15(5):482-5.
Iron deficiency in stabled Dutch warmblood foals.
Brommer H, Sloet van Oldruitenborgh-Oosterbaan MM. Department of Equine Sciences, Faculty of Veterinary Medicine, Utrecht University, The Netherlands. H.Brommer@vet.uu.nl Abstract Forty-three
Dutch Warmblood foals were divided at random into 3 rearing groups immediately after birth: a box-rest group, a box-rest with exercise group, and a pasture group. All stabled foals (box-rest and exercise groups) were fed freshly cut grass harvested from the same pastures on which the pasture group foals were grazing. Blood samples were obtained monthly for CBC and biochemical analyses. At 1-3 months of age, the foals at pasture were active but the foals in the box-rest and exercise groups were listless. Mean hemoglobin concentrations, PCVs, blood iron concentrations, and saturation of total iron binding capacity were significantly lower (P < .05) in the box-rest group (11.3+/-1.2 g/dL, 33+/-3%, 123+/-67 microg/dL, and 18+/-9%) and the exercise group (11.6+/-1.5 g/dL, 34+/-4%, 101+/-61 microg/dL, and 15+/-10%) compared with the pasture group (14.0+/-0.8 g/dL, 42+/-3%, 212+/-67 microg/dL, and 32+/-10%). Oral supplementation of iron to all foals resulted in significant increases in the values of these variables in the box-rest group and exercise group at 4-5 months of age, and the stabled foals were as active as the foals at pasture. In the pasture group, no significant changes occurred. Management practices clearly influence the iron state in young growing foals from 1 to 3 months of age, and although not a frequent cause of anaemia in the horse, an absolute deficit of body iron may occur in stabled foals fed freshly cut grass.
I should mention here that if the foals had been fed hay rather than freshly hand-cut grass there may not have been a problem. Most hay is contaminated to some extent with dirt.
A diet-related iron deficiency anaemia has never been found in an adult horse, and horses do not respond to iron supplementation with improved haemoglobin or red cell counts.
Once absorbed, there is virtually no avenue for iron excretion. Once iron is absorbed, it cycles very efficiently between haemoglobin and a few iron-containing enzymes, and storage depots for iron, primarily in the spleen and liver.
To summarise
- Iron deficiency as a cause of equine anaemia is virtually nonexistent in horses.
- Iron overload is fairly common and can contribute to anaemia in horses by causing oxidative stress.
- Deficiency of copper is common and can cause equine anaemia by interfering with recycling of iron in the body.
- Deficiencies of zinc, copper, vitamin E and selenium can compromise antioxidant defense systems and contribute to horse anaemia related to oxidative stress.
Last Updated on June 23, 2022 by Forageplus Team


